This implies origination at the apex (the ventricle, where VT originates) with propagation towards the base of the heart ("base" meaning upper right). VT? There is a "northwest" axis (between -90 and 180, with a large monophasic R-wave in aVR). Even if it is sinus tach, neither of these therapies is terribly dangerous, but they will not benefit the patient.įourth, is there any evidence from the QRS that this is SVT vs.

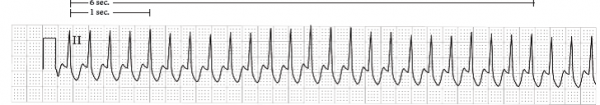
Third, assuming it is truly NOT sinus tachycardia, either adenosine at a higher dose or electrical cardioversion works well. However, this patient does have structural heart disease, so VT is not at all unlikely. Second, in most young people without structural cardiac disease, SVT is more likely. It is done with the monitor, not the 12-lead. Here are the instructions for recording Lewis leads. To diagnose sinus tachycardia, one can use Lewis leads in order to uncover hidden P-waves. If identical, then this is supraventricular (which includes sinus tachycardia). If the patient had been stable (conscious), then there would have been a few minutes to think:įirst, if one can easily find old ECGs that are in sinus rhythm, then one can compare the QRS morphology at baseline with this one in tachycardia. Thus, it is very likely that the patient has uncorrectable hypoxemia due to shunt physiology. This is especially true if there is no evidence of pulmonary edema on chest X-ray or bedside ultrasound. One might call this patient unstable because of the low saturations, but a patient with a known single ventricle is likely to have cyanotic heart disease and to have baseline O2 saturations that are very low, even on high flow O2. Thus she must be considered unstable, so use electricity! Her altered mental status may be due to hypoperfusion (shock), in spite of the normal blood pressure (non-invasive blood pressures are unreliable in sick patients). If the patient is unstable, just cardiovert with electricity. Is it Ventricular Tachycardia (VT) or SVT with aberrancy?įull interpretation is at the far bottom of the post There is a monomorphic Right Bundle Branch block pattern with QRS duration of between 140 - 160 ms (is it difficult to ascertain the exact beginning and end of the QRS) There is a regular, wide complex tachycardia at a rate of 160, with no P-waves. They did notice "clubbing" of the fingers.Ī relative was able to state in broken English "single ventricle." O2 sats were 70s and 80s on high flow O2, but there was no evidence of pulmonary edema. Her blood pressure was normal throughout the case. There were no records immediately available. She was cyanotic and minimally responsive on arrival here, and had a healed sternotomy scar. They attempted cardioversion with adenosine, unsuccessfully (dose was uncertain, thought to be 12 mg, but this would be an unusual initial dose). This case was sent by a former HCMC resident:Ī 20-something non-English speaking woman with a history of some sort of congenital heart defect collapsed at home and EMS found her with a regular wide complex tachycardia around 200 bpm.

